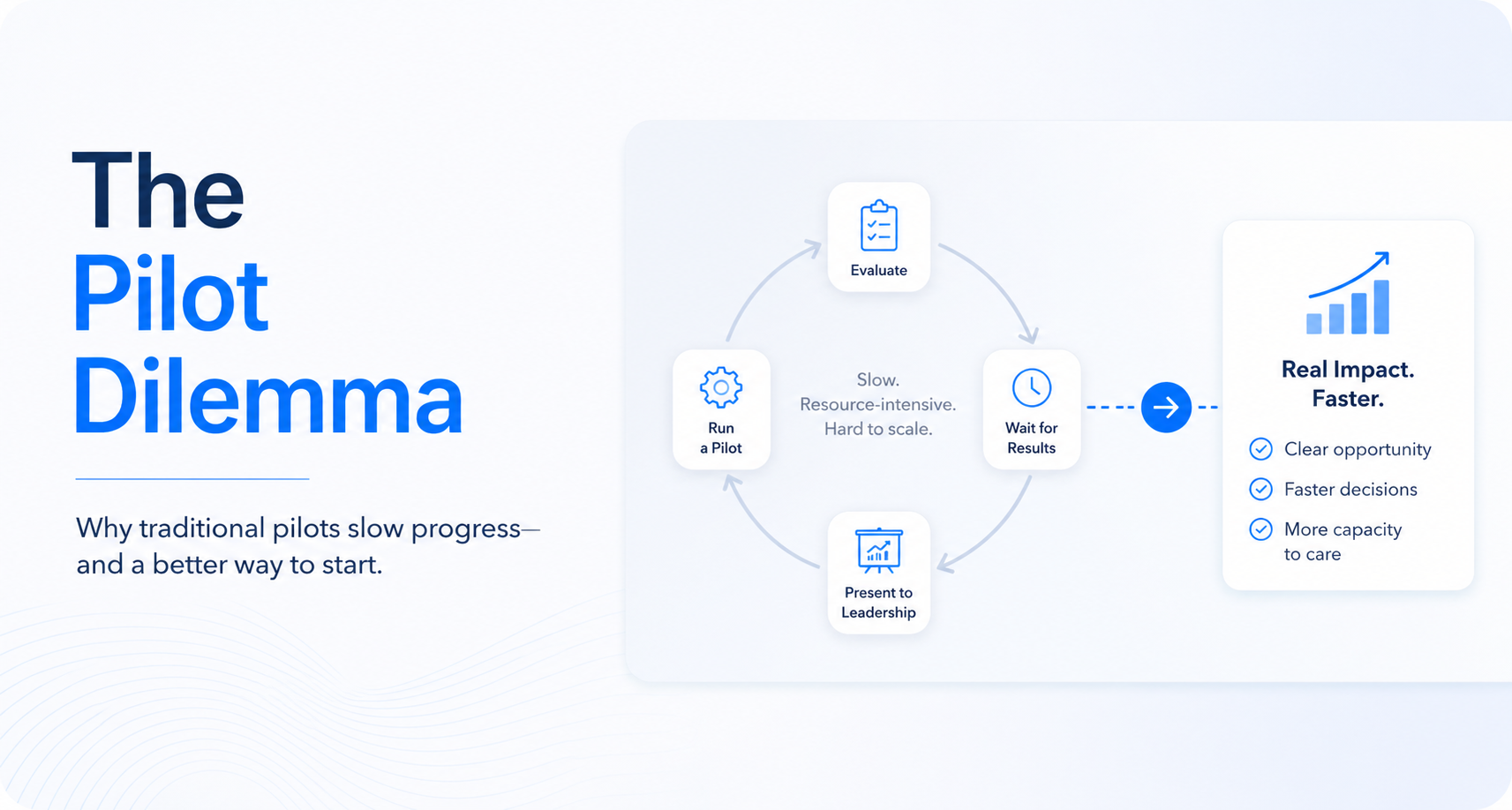
Most perioperative leaders know the routine: evaluate a vendor, run a pilot program, wait for results, present to leadership, and repeat with the next solution.
What started as a risk-management strategy has become a hard-to-break cycle. Meanwhile, surgical demand continues to rise, operating room resources remain constrained, and patients are still waiting for access to care.
This all reflects the reality of pilot fatigue in practice.
Where pilots start to break down
There is nothing inherently wrong with pilots. The logic is sound: test before committing, validate value, and make a more informed decision.
However, in practice, pilots often introduce a different kind of friction. They typically take months to complete and require significant internal effort to manage. Moreover, the results can be challenging to generalize beyond the specific environment in which they were tested.
Even after all this effort, healthcare executives often find themselves in the same position: still struggling to clearly articulate what impact the solution will deliver, when, and at what scale. Meanwhile, the operational challenges that prompted the pilot in the first place almost never get resolved.
Estimate the impact of OR intelligence on your hospital.
Calculate your impact
The burden often falls on the people closest to the problem
One of the more frustrating dynamics is that those who understand the problem best are rarely the ones in control of the budget. Perioperative leaders have firsthand experience with the inefficiencies in their hospitals. They know where time is wasted, where schedules fall apart, and where capacity is underutilized (or overutilized through overtime and late days). In many cases, they are already convinced that change is necessary.
What they need is a way to communicate their insights that will resonate with executive leadership. Unfortunately, the typical way to prove the need for change often involves presenting precise data and modeling results — luxuries that hospitals rarely have for their OR operations — or launching (you guessed it) a pilot program.
The pilot approach can be slow and resource-intensive, and it places the burden of validation on the very leaders who are already juggling day-to-day operations.
What leaders are actually trying to understand
The real question isn’t simply whether a solution works. It’s whether it will work in their environment and what kind of impact it could realistically have.
Case studies and external benchmarks only go so far. What tends to move decisions forward is a credible estimate grounded in a hospital’s own operating reality: their ORs, their case volume, their turnover times, their resource misallocation.
A more practical starting point
Before committing to a full evaluation, it helps to get a quick, directionally accurate estimate of what the opportunity could look like in your own ORs. So Apella built an Impact Calculator to make those core insights simple, accessible, and immediate.
In about a minute, hospital leaders can input a few basic details about their ORs and get an estimate of how much untapped surgical capacity may already exist within their current setup — through better utilization and higher case throughput and without adding rooms, extending hours, or increasing staffing that all drive huge costs.
It’s not meant to replace a deeper evaluation, but it provides something that’s often missing early in the process: a concrete, organization-specific starting point for discussion and evaluation.
Moving forward without getting stuck in misdirected pilots
The goal of running a pilot has always been to build confidence in a decision. But pilots aren’t the only way to get there, and, in many cases, they are not the most efficient one.
Leaders need faster, more practical ways to understand the size of the opportunity and make informed decisions without getting stuck in prolonged trial cycles.
If you’re currently assessing solutions meant to increase efficiency and throughput in the OR, a useful place to start is to quantify the opportunity and see what the improvement might yield in your own environment.
Estimate the impact of OR intelligence on your hospital.
Calculate your impact