Most healthcare leaders face a similar set of challenges:
- Expanding patient access to surgery
- Avoiding staff burnout despite a packed case schedule
- Increasing capacity to drive greater revenue
- Decreasing costs and controlling overhead
Achieving any of these objectives in isolation typically requires an expensive series of interventions that are complicated and slow to implement. Attempting to take down all four can cost tens of millions of dollars and years of major project cycles, usually overseen by pricey outside consultants.
The overarching belief is that truly transformational change is more than most hospitals can endure. This is especially true in the operating room, which remains simultaneously the biggest contributor to both health system revenue and cost, as well as some of the most expensive commercial real estate in America. However, the common assumptions behind these challenges are not entirely accurate
The false tradeoff
Many believe that increasing case volume requires more rooms, longer hours, and/or additional staff. However, most busy hospitals could boost case volume without these changes by focusing on increasing surgical throughput with the resources they already have. Typically, 23% of OR time sits unused as idle time is generally unseen and almost completely unmeasured. Factors like underutilized block time, late case releases, same-day cancellations, and small gaps between cases contribute to this idle time. The real limiting factor isn't the number of rooms; it’s the lack of visibility into available time and a plan to allocate existing resources to increase surgical throughput.

Estimate the impact of OR intelligence on your hospital.
Calculate your impact
Why the opportunity stays hidden
Even when hospital leaders suspect time is being lost, the absence of data makes it difficult to identify where and how time is lost. Three patterns consistently emerge across health systems:
Late data
EHR timestamps are entered manually, averaging 20 minutes after the event. By the time leaders see what's happening in their ORs, the opportunity to intervene has already passed.
Inaccurate case scheduling
Only 44% of cases are scheduled within 30 minutes of their actual duration. The remaining 56% result in either idle gaps that can't be filled or unplanned overtime that stresses staff. Of the cases that are over- or under-scheduled by at least 30 minutes, a staggering 29% are off by more than an hour.
Turnover and phase inefficiencies
Time outside active procedures — like prep, wrap-up, and turnover — averages 67% of OR time. For the same surgery, this can vary up to an hour across different sites. Most opportunities in ORs aren't inside the procedure itself but in these surrounding processes.
These problems aren't exceptions; they are the rule in most American hospitals. Together, they represent significant recoverable capacity of which most teams are unaware.
What recovery actually looks like
When hospitals have precise visibility into how time is allocated and utilized, teams can transform their operating rooms and relatively easily turn unused time into more cases. Blocks are released sooner, gaps are filled promptly, and turnover variability is managed in real time on a case-by-case basis. Apella customers typically see an additional two cases per OR each month — not through resource expansion, but by reclaiming available time to increase surgical throughput.
For hospitals already contemplating construction to meet rising demand, such immediate improvements to proactively optimize capacity utilization are absolutely critical to the long-term plan. While building new ORs can take years, optimizing existing capacity can begin within 30 days and drive impact at scale for decades to come.
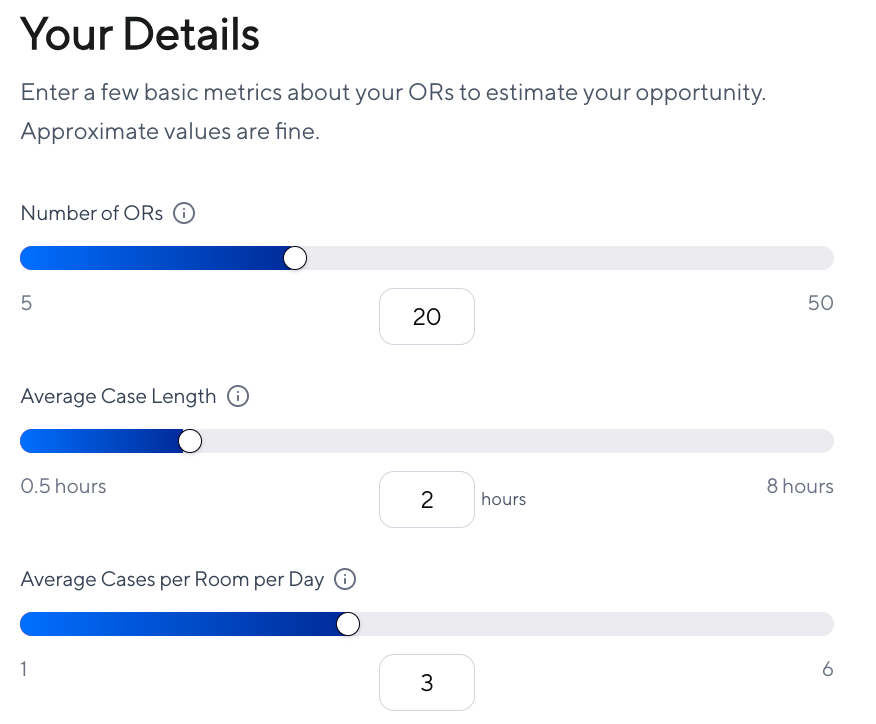
Find out what your ORs can achieve
Apella's new Impact Calculator lets healthcare leaders see their opportunity to improve case volume, surgical income, and overall efficiency in the operating room according to their own numbers — rooted in benchmarks from hospitals nationwide running on Apella.
Enter five basic metrics about your OR operations and, in seconds, get a personalized estimate of your recoverable minutes, additional cases per year, and revenue opportunity in seconds.
Estimate the impact of OR intelligence on your hospital.
Calculate your impact

